 At the moment, there is no unanimity with regards to the optimum surgical treatment of PMD and larger prospective studies will be required to form a more robust algorithm for the surgical approach of PMD individuals whose vision cannot be corrected with spectacles or contact lenses. To date, there are no large prospective interventional studies to elucidate the optimum surgical approach for advanced PMD, only case reports or case series.Ĭonclusion: Eye care practitioners need to be aware of the clinical and topographic findings of this disease, since laser refractive surgery is a contraindication. Management of PMD includes the use of contact lenses, spectacles and a wide range of surgical techniques with variable results. PMD patients are at risk of corneal perforation after minimal ocular trauma or even spontaneously. It mainly affects the inferior cornea and induces against the rule irregular corneal astigmatism. Results: PMD is a rare ectatic disorder of the cornea that may resemble keratoconus especially at the early stages. Materials and Methods: Literature review via PubMed, Mendeley, Scopus and Google Scholar. After surgery you should avoid any heavy lifting and strenuous activity for 1 month.Purpose: To describe the clinical features of Pellucid Marginal Degeneration (PMD) and to give an overview of current treatment options. It is essential to take your drops as prescribed to maintain function of the transplant. You will also take steroid drops that will be gradually reduced over time to 1 drop per day, but you will likely continue permanently. You will start taking antibiotic drops 3 days prior to surgery and continue until the bottle is empty. You should ensure that you understand all instructions provided. What do I need to do before and after surgery? Visual improvement with DMEK and DSAEK usually occurs in a few weeks. Healing of a full thickness transplant can take up to 1 year. Best possible vision is achieved once wounds have fully healed and stitches removed. You can expect to have moderate discomfort, irritation and redness for up to 3 weeks. McCarthy will inform you if you are at an increased risk for any of the above complications. Fortunately, the majority of complications are treatable and have good outcomes. Other less common complications include bleeding, swelling, glaucoma and retinal detachment. The primary risks are rejection and infection which are minimized with the use of antibiotic and steroid drops. McCarthy will go over your individual case with you.Ĭorneal transplants remain a serious surgery with certain risks that you should be aware of. However, it can vary from 50% to 95% depending on the condition being treated. Today, the overall success rate is above 85%. The success rate of corneal transplants has drastically improved in the last 30 years. On treatment day, you will be instructed to arrive at the hospital about 1.5 hours in advance and the surgery will take approximately 30 minutes. Partial thickness transplants replace only certain layers, leave the rest intact and use fewer stitches. The transplant is then secured using tiny stitches about 1/3 the thickness of a human hair. With full thickness transplants, the damaged cornea is removed through a process called trephination and replaced with a donor cornea. All donated corneas are verified to be healthy, clear and appropriate for you.Ĭorneal transplants are generally done under local anaesthetic. over 500 people require a corneal transplant which uses tissue generously gifted by registered organ donors who have passed away. How do I know if I would benefit from a corneal transplant?Ī corneal transplant is normally indicated once your damaged cornea interferes with your ability to do activities important to you or is causing significant constant pain not treatable by other means.Įvery year in B.C. 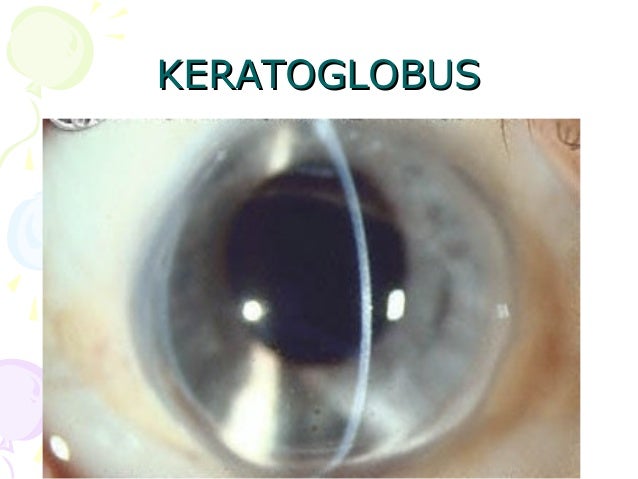
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
